NewsMakers
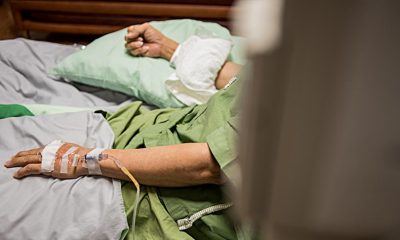
Young Filipinos more susceptible to illness despite health awareness, says Manulife study
According to Rahul Hora, Manulife Philippines president and chief executive officer, many young Filipinos are facing a rise in illnesses and lifestyle-related issues despite health awareness. “This gap between awareness and action implies that mere knowledge isn’t sufficient. We must find solutions to these real-world barriers preventing young people from practicing healthier lifestyles.”

Financial security, susceptibility to illnesses, and lack of health awareness are factors that influenced the behavior of Filipinos in adopting healthier lifestyles. This is according to a study conducted by Manulife Philippines entitled “In Wellness and In Health” which delves into the landscape of health, well-being and financial preparedness in the Philippines.
Conducted to a total 1,000 Filipino male and female consumers across four age groups (18-29; 30-39; 40-49; and 50-55), and different income groups, the study found out that 86% of respondents believe their health is determined by their lifestyle choices. This same percentage also cited barriers that prevent them from having healthy lifestyles.
According to Rahul Hora, Manulife Philippines president and chief executive officer, many young Filipinos are facing a rise in illnesses and lifestyle-related issues despite health awareness. “This gap between awareness and action implies that mere knowledge isn’t sufficient. We must find solutions to these real-world barriers preventing young people from practicing healthier lifestyles.”
The study says 33% of Filipinos, prominently in the lower income households, admit their current lifestyle is unhealthy, with younger Filipino adults at age range 18 to 29 get sick more often than other age groups, despite health awareness. It was also noted in the survey that among all respondents, the average number of sick days a year is 2.7 times. However, for those in the 18 to 29 age group who get sick more often, the number rose to an average of 3.4 times a year.
This may be the result of unhealthy diet, stress, and the lack of sleep and exercise among young Filipinos in the 18 to 29 age bracket, compared with other age groups. According to 68% of respondents, the reason for lower exercise rates was a perception that following a regular exercise routine is expensive.
The lack of proper sleep and exercise, as well as the tendency to neglect their overall health, can make younger Filipinos susceptible to illness. This age group is also more reluctant to changing their lifestyles due to a perceived “fear of missing out.” They spend a huge chunk of time nurturing their social lives, and may be less willing to change their habits for a healthier lifestyle due to perceived costs and inconvenience.
Hora said young Filipinos need the support they can get to better translate health and wellness information into everyday habits, including taking necessary steps toward achieving financial security.
Meanwhile, to prevent illness, a healthy diet is considered as the healthy lifestyle to follow. But, in contrast, three in every 10 Filipino respondents admit their current lifestyles are unhealthy, and half of the respondents claimed that majority of their meals are not healthy.
Lack of knowledge and misinformation about health alter Filipinos’ perceptions of the need for a healthy lifestyle. Forty six percent of respondents believe that healthy meals are less appetizing while 35% share that they are more difficult to prepare and find. The survey also found out that 25% believe critical illnesses can only afflict older Filipinos, while 21% think eating habits and nutrition have very little or no impact on children’s mental development.
Hora said the survey underscores a critical gap between awareness of the importance of a healthy diet and its actual implementation among Filipinos. “Misconceptions and perceived barriers such as cost, taste, and preparation difficulty continue to hinder healthier lifestyle choices. It is important to address these issues through education and accessibility to ensure better health outcomes for all.”
The survey found out that Filipinos remain financially unprepared for medical emergencies as a significant portion of medical expenses, about 41%, still comes out-of-pocket, mainly from personal savings. This highlights a gap between the perceived adequacy of health coverage and the financial reality faced during actual medical emergencies, putting a considerable burden on individuals and families.
The survey also reveals a stark difference in savings for medical expenses across different age
groups. On average, respondents have set aside PhP62,000 for future medical needs such as emergency services, hospitalization, and preventive healthcare.
However, the survey says younger Filipinos aged 18-29 have saved significantly less, with an average of only PhP38,000. This disparity suggests that younger individuals might be less prepared to handle unexpected medical costs. Additionally, respondents believe they will need to save approximately PhP571,000 to cover potential medical expenses over the next 10 years, highlighting a substantial gap between current savings and future financial needs.
“These key findings further prove that, when we talk about healthcare and well-being, we must understand where knowledge and behavioral gaps are coming from,” Hora said.
Hora encourages Filipinos to take more concrete steps toward embracing healthier lifestyles – from improving dietary habits to nurturing overall well-being. For financial priorities, Manulife can be a trusted partner through its broad range of health and life protection plans to secure their future and help them live better every day. By addressing both health and financial preparedness, Filipinos can build a more resilient foundation for managing their healthcare need.
NewsMakers
Common drug class may increase risk of heart disease
The risk of cardiovascular disease increased in line with how much anticholinergic medication the participants used each year. Those with the highest exposure had a 71 per cent higher risk of a cardiovascular event than people who did not use anticholinergic medication at all.

People who use drugs with anticholinergic effects, including certain antidepressants, drugs for urinary incontinence and common antihistamines, are at higher risk of developing cardiovascular disease.
This is shown in a study from Karolinska Institutet published in BMC Medicine.
Anticholinergic drugs reduce the effect of the neurotransmitter acetylcholine and are commonly prescribed to middle-aged and older people. This large group of drugs includes antihistamines used for allergic conditions, anxiety or insomnia, drugs for urinary incontinence, and certain antidepressants, where tricyclic antidepressants have a strong anticholinergic effect, whereas SSRIs have a weaker effect. A high cumulative use of these drugs, referred to as anticholinergic burden (see fact box), has previously been linked to impaired cognitive ability.
May affect heart regulation
The new study suggests that the drugs may also affect the parasympathetic nervous system and thereby the regulation of the cardiovascular system. The results show that it may be important to monitor the total drug burden in everyday clinical practice.
The study included more than 500,000 people in Stockholm, Sweden, who were 45 years of age or older and had no prior cardiovascular disease, except for hypertension, at the start of the study. The researchers followed the participants for up to 14 years and analysed how the use of anticholinergic drugs was associated with the development of cardiovascular disease.
“Many of these drugs are used by older people and by people with multiple medical conditions. We wanted to investigate whether the total exposure had any significance for the risk of developing cardiovascular disease over time,” says Nanbo Zhu, postdoctoral researcher at the Department of Neurobiology, Care Sciences and Society, Karolinska Institutet.
71 per cent higher cardiac risk
The study showed that the risk of cardiovascular disease increased in line with how much anticholinergic medication the participants used each year. Those with the highest exposure had a 71 per cent higher risk of a cardiovascular event than people who did not use anticholinergic medication at all. The association was seen for all types of cardiovascular disease but was particularly clear for heart failure and various forms of arrhythmia.
“Our results indicate that the cumulative drug burden can affect heart regulation, not only in the short term but also over the long term. This does not mean that the drugs should always be avoided, but that exposure should be monitored carefully,” says Hong Xu, assistant professor at the Department of Neurobiology, Care Sciences and Society.
The researchers point out that the study is observational, meaning it cannot establish a causal relationship. Other factors, such as underlying diseases, may also influence the associations.
The work was carried out within the Stockholm CREAtinine Measurements project in collaboration between several research groups at Karolinska Institutet and Region Stockholm. The study was funded by the Swedish Research Council, the Center for Innovative Medicine Foundation, and other foundations. Some researchers report assignments for the pharmaceutical industry, which are disclosed in the scientific publication.
NewsMakers
Mindfulness practices found to significantly reduce depression symptoms, especially for those with early-life adversity
Mindfulness interventions help by regulating our emotions better when different challenges come up. For someone who has experienced childhood neglect or abuse, mindfulness training can help us make sense of that and respond skillfully to this moment in time.

A new study reveals that mindfulness practices may significantly reduce depression symptoms, particularly in people who have experienced early-life adversity, such as childhood abuse and neglect.
Led by Eric Loucks, professor of medicine, epidemiology, and of behavioral and social sciences and director of the Mindfulness Center at Brown, the study enrolled 201 participants, 101 of whom were randomized into the Mindfulness-Based Blood Pressure Reduction Program, while 100 were randomized into an enhanced usual care control, which included home blood-pressure monitors, physician access and health-education materials. Researchers also had a measure of participants’ early-life adversity, particularly their exposure to abuse or neglect.
Loucks and his team followed participants for six months to assess changes in blood pressure, health behaviors and mental health, finding that those in the mindfulness program showed significant improvements in their depression symptoms. Additionally, participants who experienced childhood neglect showed greater improvements in depression symptoms than those who had not. A similar, though less pronounced, trend was observed among people with a history of childhood abuse.
“In this program, that was primarily designed to lower blood pressure while addressing whole-person health, we also saw that mental well-being, particularly around depression symptoms, improved in participants that went through the program,” Loucks said. “The findings suggest that cultivating mindful self-regulation skills–such such as self-awareness, attention control and emotion regulation–may help interrupt maladaptive patterns shaped by past experiences.”
Over the last 15 years, Loucks has been studying social determinants of health such as early-life adversity and its impacts on cardiovascular health, body mass index and blood pressure. “I came to a point where I wanted to not just document it, but do something about it, and I wondered if mindfulness training might help,” he said. “I’d gone through a lot of mindfulness training myself outside of work and started to get trained up in mindfulness programs that are specific to health contexts.”
Loucks began to study the Mindfulness-Based Stress Reduction program, running it through two clinical trials that were funded by the NIH and finding that it reduced blood pressure in both trials. He also wanted to look at the intervention from a whole-person perspective.
“If we look at everyday folks out in the world, those that had exposure to early life adversity, like abuse and neglect, tend to have worse mental health and also worse cardiovascular health,” Loucks said. “Mindfulness interventions help by regulating our emotions better when different challenges come up. For someone who has experienced childhood neglect or abuse, mindfulness training can help us make sense of that and respond skillfully to this moment in time.”
Loucks discussed this work during a keynote address at the U.S. DOHaD Society this year. “It felt like a coming-home moment to see that this intervention, originally developed to address psychosocial factors that influence health, had even stronger effects among people with early-life adversity, particularly on depression,” he said. “It’s been about a 15-year arc of research that culminated in these findings.”
NewsMakers
High-fiber diet linked to reduced risk of heart disease in night shift workers
A moderate intake of about 19 grams of fibre per day was linked to a lower risk for those who worked night shifts regularly. For those who worked night shifts sporadically, about 15 grams was enough. The current recommendation for adults is about 25 grams of dietary fibre per day.

People who work at night have a higher risk of coronary artery disease, a type of heart disease. A new study suggests that a higher fibre intake in the diet may help reduce this risk. The study included over 220,000 adults in the UK and is published in the European Journal of Epidemiology.
The human body is built to sleep at night. This means that working during the night goes against this natural pattern, and can place additional strain on the body, including the heart. Previous research has linked night work to an increased risk of coronary artery disease. Since night work is often unavoidable, the researchers wanted to investigate whether certain dietary habits might have a protective effect.
More fibre associated with lower risk
The researchers used data from 220,000 adults in the UK Biobank (2006–2010) and divided the participants into three groups:
- Day workers
- Shift workers who worked night shifts sporadically
- Regular night shift workers
The participants had completed a detailed questionnaire about their dietary habits. During a follow-up after about 12 years, it was found that night shift workers who consumed little fibre in their diet had a higher risk of coronary artery disease than those who consumed more fibre.
“A moderate intake of about 19 grams of fibre per day was linked to a lower risk for those who worked night shifts regularly. For those who worked night shifts sporadically, about 15 grams was enough. The current recommendation for adults is about 25 grams of dietary fibre per day,” says Diana Nôga, lead author and researcher at Uppsala University.
The researchers stress that the figures from the study are not official dietary recommendations. But they do show a pattern in this UK study: a higher dietary fibre intake was linked to a lower risk of heart disease among night shift workers.
“The link between fibre and a lower risk of heart disease is not just because those who eat more fibre generally have a healthier lifestyle. We know this because we adjusted for various lifestyle factors in the analysis. One possible explanation, supported by previous research, is that fibre in the diet can improve intestinal flora and also reduce lipids, which can be particularly good for the heart in people who work at night,” says Christian Benedict, senior author of the study and Professor of Pharmacology at Uppsala University.
Dietary fibre can support heart health
According to the researchers, an increased intake of fibre-rich foods such as whole grains, vegetables, fruit, legumes and lentils may be a simple way to improve heart health for night shift workers. However, this requires that you do not have any medical obstacles to doing this, such as chronic gastrointestinal diseases.
“Dietary changes should be seen as a complement to, not a substitute for, other heart health-promoting habits such as not smoking, remaining physically active, and getting enough sleep,” says Diana Nôga.
-

 NewsMakers3 weeks ago
NewsMakers3 weeks agoCreativity feels great — until tomorrow
-

 NewsMakers3 weeks ago
NewsMakers3 weeks agoHigh-fiber diet linked to reduced risk of heart disease in night shift workers
-

 NewsMakers3 weeks ago
NewsMakers3 weeks agoSleeping in on weekends may help boost teens’ mental health
-

 Wellness3 weeks ago
Wellness3 weeks agoExercise to treat depression yields similar results to therapy
-

 Destinations3 weeks ago
Destinations3 weeks agoChecking the charm of Baguio City’s Café by the Ruins
-

 NewsMakers3 weeks ago
NewsMakers3 weeks agoTwo types of underconfidence linked to anxiety and gender
-

 Wellness3 weeks ago
Wellness3 weeks agoAerobic exercise may be most effective for relieving depression/anxiety symptoms
-

 NewsMakers2 weeks ago
NewsMakers2 weeks agoMindfulness practices found to significantly reduce depression symptoms, especially for those with early-life adversity