NewsMakers
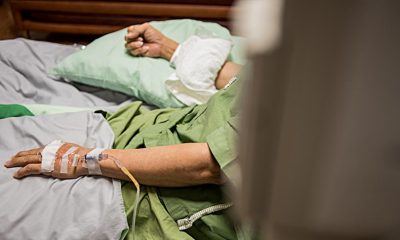
What you should know about IBD
Two common conditions are irritable bowel syndrome (IBS) and inflammatory bowel disease (IBD). They’re often confused for one another, but these are actually two different GI disorders.

It may not be something you like to talk about, but if you have gastrointestinal (GI) problems, your symptoms may be far more common than you think. According to data from the American Gastroenterological Association, 60-70 million people living in the United States have gut health concerns.
Two common conditions are irritable bowel syndrome (IBS) and inflammatory bowel disease (IBD). They’re often confused for one another, but these are actually two different GI disorders.
IBS is a syndrome; it is defined by a group of symptoms, does not cause inflammation and rarely requires hospitalization or surgery. IBD, on the other hand, is an umbrella term used to describe disorders that cause chronic inflammation of your GI tract.
The disease is more common than you may realize; a study led by the Crohn’s & Colitis Foundation found nearly 1 in 100 people living in the U.S. have IBD. The two most common forms of IBD are Crohn’s disease and ulcerative colitis.
Understanding IBD Symptoms
Because it poses serious health risks and can cause permanent damage to your intestines, it’s important to be aware of what IBD is and recognize the symptoms. Your primary care doctor or gastroenterologist can help if you have concerns about these symptoms:
- Intense, crampy pain that doesn’t go away in a day or two or has been present on and off for weeks or longer
- A notable change in bowel movement frequency, whether more or less often
- Frequent diarrhea over several weeks, or loose stools multiple times a day
- Frequent constipation, or constipation alternating with diarrhea
- Urgency on a regular basis or inability to hold back the bowel movement before reaching the bathroom
- Blood with bowel movements
- Mucus in your stool regularly or paired with pain or other symptoms
- Always feeling as though you aren’t fully emptying your bowels
Other symptoms that may have a variety of causes but need extra attention especially if you notice them along with any of the symptoms above include pain outside of the gut, fatigue, loss of appetite and weight loss. In addition, children with IBD may have delays in growth and the onset of puberty.
Diagnosing IBD
No single test can confirm a Crohn’s or ulcerative colitis diagnosis. Your medical history and information obtained from diagnostic testing can exclude other potential causes of your symptoms, since gastrointestinal symptoms are common and can have a variety of causes.
Your first tests will likely include blood and stool laboratory tests. Further testing could include imaging studies of your gastrointestinal tract or a look inside your GI tract through an endoscope.
Identifying Treatment Options
Once an IBD diagnosis is confirmed, you can partner with your doctor to manage your disease. Treatment plans are highly personalized, as what works for one person may not for another. Medication and managing your diet and nutrition are two common treatment recommendations. In some cases, surgery can help improve your quality of life.
Clinical trials may also be an option for treating your IBD. Through clinical trials, researchers find new ways to improve treatments and quality of life. In fact, clinical trials represent the final stages of a long and careful research process to make new and improved treatment options for patients available.
However, an important part of clinical trials for IBD is patient participation. Without the enrollment of patients in clinical trials, new treatment options for IBD can be delayed or never become available.
Equally important to this process is having a diverse representation of patients that considers race, age or other categories. This helps researchers develop treatments that meet the needs of a vast IBD patient community.
If you’re interested in participating in a clinical trial, ask your doctor to help you find a trial that is right for you, and visit crohnscolitisfoundation.org to learn more about IBD and treatment options, including clinical trials.
NewsMakers
Drinking any amount of alcohol likely increases dementia risk
Even light drinking—generally thought to be protective, based on observational studies—is unlikely to lower the risk, which rises in tandem with the quantity of alcohol consumed.

Drinking any amount of alcohol likely increases the risk of dementia, suggests the largest combined observational and genetic study to date, published online in BMJ Evidence Based Medicine.
Even light drinking—generally thought to be protective, based on observational studies—is unlikely to lower the risk, which rises in tandem with the quantity of alcohol consumed, the research indicates.
Current thinking suggests that there might be an ‘optimal dose’ of alcohol for brain health, but most of these studies have focused on older people and/or didn’t differentiate between former and lifelong non-drinkers, complicating efforts to infer causality, note the researchers.
To try and circumnavigate these issues and strengthen the evidence base, the researchers drew on observational data and genetic methods (Mendelian randomisation) from two large biological databanks for the entire ‘dose’ range of alcohol consumption.
These were the US Million Veteran Program (MVP), which includes people of European, African, and Latin American ancestry, and the UK Biobank (UKB), which includes people of predominantly European ancestry.
Participants who were aged 56–72 at baseline, were monitored from recruitment until their first dementia diagnosis, death, or the date of last follow-up (December 2019 for MVP and January 2022 for UKB), whichever came first. The average monitoring period was 4 years for the US group, and 12 for the UK group.
Alcohol consumption was derived from questionnaire responses—over 90% of participants said they drank alcohol—and the Alcohol Use Disorders Identification Test (AUDIT-C) clinical screening tool. This screens for hazardous drinking patterns, including the frequency of binge drinking (6 or more drinks at a time).
In all, 559,559 participants from both groups were included in observational analyses, 14,540 of whom developed dementia of any type during the monitoring period:10,564 in the US group; and 3976 in the UK group. And 48,034 died: 28,738 in the US group and 19,296 in the UK group.
Observational analyses revealed U-shaped associations between alcohol and dementia risk: compared with light drinkers (fewer than 7 drinks a week) a 41% higher risk was observed among non-drinkers and heavy drinkers consuming 40 or more drinks a week, rising to a 51% higher risk among those who were alcohol dependent.
Mendelian randomisation genetic analyses drew on key data from multiple large individual genome-wide association studies (GWAS) of dementia, involving a total of 2.4 million participants to ascertain lifetime (rather than current) genetically predicted risks.
Mendelian randomisation leverages genetic data, minimising the impact of other potentially influential factors, to estimate causal effects: genomic risk for a trait (in this case, alcohol consumption) essentially stands in for the trait itself.
Three genetic measures related to alcohol use were used as different exposures, to study the impact on dementia risk of alcohol quantity, as well as problematic and dependent drinking.
These exposures were: self-reported weekly drinks (641 independent genetic variants); problematic ‘risky’ drinking (80 genetic variants); and alcohol dependency (66 genetic variants).
Higher genetic risk for all 3 exposure levels was associated with an increased risk of dementia, with a linear increase in dementia risk the higher the alcohol consumption.
For example, an extra 1-3 drinks a week was associated with a 15% higher risk. And a doubling in the genetic risk of alcohol dependency was associated with a 16% increase in dementia risk.
But no U-shaped association was found between alcohol intake and dementia, and no protective effects of low levels of alcohol intake were observed. Instead, dementia risk steadily increased with more genetically predicted drinking.
What’s more, those who went on to develop dementia typically drank less over time in the years preceding their diagnosis, suggesting that reverse causation—whereby early cognitive decline leads to reduced alcohol consumption—underlies the supposed protective effects of alcohol found in previous observational studies, say the researchers.
They acknowledge that a principal limitation of their findings is that the strongest statistical associations were found in people of European ancestry, because of the numbers of participants of this ethnic heritage studied. Mendelian randomisation also relies on assumptions that can’t be verified, they add.
Nevertheless, they suggest that their findings “challenge the notion that low levels of alcohol are neuroprotective.”
And they conclude: “Our study findings support a detrimental effect of all types of alcohol consumption on dementia risk, with no evidence supporting the previously suggested protective effect of moderate drinking.
“The pattern of reduced alcohol use before dementia diagnosis observed in our study underscores the complexity of inferring causality from observational data, especially in ageing populations.
“Our findings highlight the importance of considering reverse causation and residual confounding in studies of alcohol and dementia, and they suggest that reducing alcohol consumption may be an important strategy for dementia prevention.”
NewsMakers
Distribution of fat could influence cancer risk, study suggests
Obesity is usually measured using body mass index (BMI), but growing evidence – particularly from heart health research – suggests that BMI alone doesn’t capture the full picture when it comes to obesity-related health risks. However, the role of fat distribution in cancer risk has been relatively unexplored.

How fat is distributed in people’s bodies could make a difference to their risk of certain cancers, according to new research led by the University of Bristol. The international study is published in the Journal of the National Cancer Institute (JNCI).
Scientists have already shown that having obesity increases a person’s risk of developing certain cancers. Obesity is usually measured using body mass index (BMI), but growing evidence – particularly from heart health research – suggests that BMI alone doesn’t capture the full picture when it comes to obesity-related health risks. However, the role of fat distribution in cancer risk has been relatively unexplored.
Researchers in Bristol’s Integrative Cancer Epidemiology Programme (ICEP) investigated whether body fat at different locations across the body influences the risks of 12 obesity-related cancers – endometrial, ovarian, breast, colorectal, pancreas, multiple myeloma, liver, kidney (renal cell), thyroid, gallbladder, oesophageal adenocarcinoma, and meningioma.
They used a technique known as Mendelian randomisation, which uses statistics, computing and the natural variations in people’s genetics to identify patterns in large health data sets.
The team found that fat distribution appears to influence cancer risk – but the relationship varies by cancer type. For some cancers, where fat is stored in the body seems more important than how much is stored; for others, the reverse is true; and, for some, both matter. In cancers where distribution is important, the specific locations of body fat driving this seem to differ by cancer, meaning the overall picture is quite complex.
Lead author, Dr Emma Hazelwood, who recently completed her PhD at the University of Bristol, explained: “These findings support the growing consensus that BMI, while useful for population-level trends, may be too simplistic for assessing individual health risks.
“Our results tell us that there is no ‘one-size-fits-all’ when it comes to cancer, meaning a more tailored approach to cancer prevention in people with obesity could be most effective.”
The paper’s findings fit with recent calls for change, including the 2024 European Association for the Study of Obesity framework and the Lancet Commission on the future of obesity, which have emphasised that BMI is a flawed diagnostic tool and that fat distribution matters.
In the future, a better understanding of how fat distribution across the body affects cancer risk could help identify those most at risk and guide more personalised approaches to obesity treatment and cancer prevention.
The research team recommend further work is needed, using different approaches and studying non-European populations.
Dr Hazelwood added: “It is vital to understand the biological mechanisms that underpin these associations – particularly how and why different fat depots affect cancer development. In the longer term, we need to explore how obesity treatments – whether lifestyle or drug-based – influence these risk pathways.”
Dr Julia Panina, Head of Research Funding at World Cancer Research Fund, added: “Our evidence-based Cancer Prevention Recommendations highlight the role of maintaining a healthy weight to reduce cancer risk. While this remains essential, growing scientific evidence shows that body composition – particularly how fat is distributed throughout the body – is also a crucial factor.
“With support from our fantastic donors, we were able to co-fund the University of Bristol’s excellent team whose findings will help direct this exciting area towards possible new cancer prevention and treatments.”
This study was funded by the World Cancer Research Fund (WCRF UK) and Cancer Research UK (Integrative Cancer Epidemiology Programme). This work was carried out at the MRC Integrative Epidemiology Unit (MRC IEU), which is supported by the Medical Research Council (MRC) and the University of Bristol.
NewsMakers
Forget materialism, a simple life is happier: research
The commitment to simple living, or ‘voluntary simplicity’ as it is formally known, leads to wellbeing through providing more opportunities for personal interaction and social connection than conventional contexts of exchange, such as community gardens, sharing resources, and peer-to-peer lending platforms.

In an age where billionaires and conspicuous consumption are increasingly on display, new Otago-led research shows a simple life really is a happier life.
The study led by University of Otago – Ōtākou Whakaihu Waka Department of Marketing researchers has recently been published in the Journal of Macromarketing.
After setting out to understand the relationship between consumption and wellbeing, the researchers found people are happier and more satisfied when adopting sustainable lifestyles and resisting the temptations of consumerism.
They analysed data from a representative sample of more than 1000 New Zealanders, made up of 51 per cent men and 49 per cent women, with a median age of 45 and a median annual household income of $50,000.
They found the commitment to simple living, or ‘voluntary simplicity’ as it is formally known, leads to wellbeing through providing more opportunities for personal interaction and social connection than conventional contexts of exchange, such as community gardens, sharing resources, and peer-to-peer lending platforms.
Women are more likely to adopt a simple life than men, although more research is needed to understand why.
Co-author Associate Professor Leah Watkins says consumer culture promotes happiness as being typically associated with high levels of income and the capability it affords to acquire and accumulate material possessions.
“However, research is clear that attitudes to, and experiences of, materialistic approaches to life do not lead to increases in happiness or wellbeing. Nor do they lead to sustainable consumption necessary for planetary health.”
Between 2000 and 2019, global domestic material consumption increased by 66 per cent, tripling since the 1970s to reach 95.1 billion metric tons.
Growing consumer affluence and higher living standards have resulted in warnings of alarming trends of environmental degradation from human consumption.
This, coupled with global warming and post-pandemic health and financial anxieties, has led researchers and policymakers to call for a better understanding of the links between simple consumer lifestyles and wellbeing.
But co-author Professor Rob Aitken says this isn’t a case of just throwing out all your worldly possessions.
“It’s not directly the commitment to material simplicity that leads to wellbeing, but the psychological and emotional need fulfilment that derives from relationships, social connection, community involvement and a sense of living a purposeful and meaningful life.
“In a world where billionaire weddings are treated like state occasions and private yachts are the new status symbols, voluntary simplicity offers a quiet, powerful counter-narrative — one that values enough over excess, connection over consumption, and meaning over materialism.”
-

 NewsMakers3 weeks ago
NewsMakers3 weeks agoUnderstanding hypertrophic cardiomyopathy
-

 Pet Care3 weeks ago
Pet Care3 weeks agoBack-to-school season can be ruff on pets
-

 NewsMakers3 weeks ago
NewsMakers3 weeks agoPlant-based nutrient improves immune cells’ ability to fight cancer
-

 Home Care3 weeks ago
Home Care3 weeks agoExplore the benefits of a bathroom upgrade
-

 Nutrition3 weeks ago
Nutrition3 weeks agoProtein-packed sweet treats
-

 Nutrition3 weeks ago
Nutrition3 weeks agoPower your summer with 100% orange juice
-

 Destinations2 weeks ago
Destinations2 weeks agoFinding Neverland in London
-

 NewsMakers3 weeks ago
NewsMakers3 weeks agoForget materialism, a simple life is happier: research