NewsMakers
Urgent action needed to counter major threat to life like Covid-19 in conflict zones
Plans to prevent and respond to the virus must urgently move forward before it gains a foothold in conflict zones.
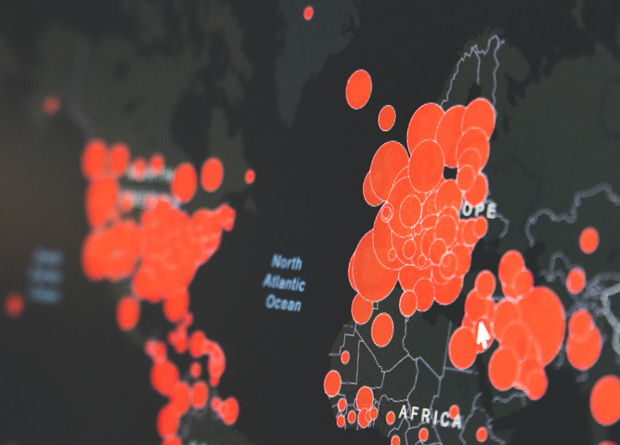
It will be nearly impossible to fight COVID-19 in countries already devastated by conflict unless a concerted response by states and humanitarian organizations is launched immediately, the International Committee of the Red Cross (ICRC) has warned. Plans to prevent and respond to the virus must urgently move forward before it gains a foothold in conflict zones.
COVID-19 represents a major threat to life in countries with strong health systems. But the threat is even greater in places where health systems have been ravaged by war, where people uprooted by conflict live in close proximity, and where life-saving resources like clean water, soap and medicine are in short supply.
Additionally, health systems weakened by conflict have reduced capacity for detection, management and the follow-up of cases of sickness, which in turn increases the risk of transmission.
COVID-19 has overwhelmed advanced health care systems. Many of the places where we work lack even basic health care infrastructure, let alone intensive care capacity. Our fear is that unless urgent action is taken to curb the spread of the virus, it will devastate some of the world’s most vulnerable communities,” said Peter Maurer, President of the International Committee of the Red Cross.
The ICRC fears the worst for people in prisons and displacement camps around the world. Health systems in conflict zones in places such as Syria, Yemen, South Sudan, northeast Nigeria, and Afghanistan are simply not prepared to handle a flood of COVID-19 cases without a surge in support.
An immediate and concerted response by states and humanitarian organizations is vital. COVID-19 does not have to be catastrophic for war-torn countries with weakened healthcare systems, but it does require the international community to scale up support. Last week the International Red Cross and Red Crescent launched an appeal for 800 million Swiss francs, a call for States to boost resources for countries with limited capacity to respond to this urgent threat.
In displacement camps, physical distancing is not possible, and we fear it will be impossible to stop the spread of coronavirus once it enters a camp. Indeed, we fear the virus will spread rapidly and viciously, straining the medical response. Containment will be difficult, as it is harder to trace and isolate suspected cases when people flee their homes due to violence.
Warfare has not stopped because of the virus, and victims of conflict still need and deserve assistance.
“Our work helping victims of conflict is still needed even amid an increased response to the virus. This work is made extra difficult because of the scale of this current pandemic, and the necessary and vital measures countries are now taking to contain it, such as movement restrictions of people and goods. To avoid a catastrophe, governments and other armed actors in conflict theaters must facilitate the work of humanitarians as a priority. Viruses know no borders: this is a global problem which will only be solved by global action,” said President Maurer.
Even as the ICRC continues its work in places of war, it is re-orienting its activities to try to prevent and assist with the COVID-19 pandemic, often in close collaboration with National Red Cross and Red Crescent Societies and the IFRC. Some of the ICRC’s COVID-19 response includes:
In Afghanistan and Myanmar, ICRC’s work in prisons and in support of health systems is focusing on COVID-19 preparedness, detection, and preventive procedures. We are also creating a rapid response plan with isolation measures, hygiene improvement and protective materials.
In Armenia, the ICRC recently donated soaps and disinfectant products to medical units of the country’s 12 detention centers. We also provided infrared thermometers to four penitentiaries.
In Burkina Faso, we are running radio spots about COVID-19. We continue to improve access to clean water and soap in areas affected by violence, and distribute soap and gel in places of detention.
In Colombia, the ICRC over the next three months will support the refurbishment of lavatories and the provision of hygiene materials in 20 detention centers to restrain COVID-19.
In the Democratic Republic of Congo, we are helping the hospitals we support to set up quarantine measures, training health care staff in suspected case isolation, and implementing infection prevention control measures in health facilities and places of detention visited by the ICRC.
In El Salvador, we are distributing soap to detainees to assist with hand washing.
In Gaza, the ICRC has donated 500 mattresses and 1,000 blankets for people in quarantine. It has also donated 43 infrared thermometers to health authorities to help screening suspected cases.
In Iraq, we have donated soap and disinfectant, protective equipment like gloves, goggles and gowns and thermometers to 13 places of detention housing 22,000 detainees. We’ll soon donate to another 11 institutions holding 20,000 detainees, including materials for handwashing and chlorine spray.
In Mexico, the ICRC and Mexican Red Cross are distributing water, hygiene kits and information on the virus to help prevent its spread.
In Lebanon, the ICRC runs an emergency ward at the Rafik Hariri University Hospital – where COVID-19 cases are being treated.
In Somalia, we provided tents for isolation to the Mogadishu hospital we support and are implementing a surveillance system to monitor suspected cases at clinics supported by the Somali Red Crescent. We are also providing hygiene items in places of detention and giving soap, chlorine tabs and hygiene information on COVID-19 to more than 120,000 households.
In Sudan, we are repairing dozens of handpumps and distributing soap to tens of thousands of displaced people, and helping government health agencies to stock gloves, gowns and disinfectant.
In Syria, in Al Hol Camp, our field hospital remains operational and our team has started to take all necessary and preventive measures to protect the patients against COVID-19.
NewsMakers
Study finds low-dose eye drops successful in managing adult myopia for 24 hours
A single low-dose atropine eye drop can produce daylong effects in managing myopia, or nearsightedness.

Groundbreaking research from the University of Houston shows that a single low-dose atropine eye drop can produce daylong effects in managing myopia, or nearsightedness, which affects roughly one-third of U.S. adults.
Professor of Optometry Lisa Ostrin and postdoctoral researcher Barsha Lal are reporting that even one drop in the eye of low-dose atropine (0.01%–0.1%) produces clear changes in pupil size and focusing ability that persist for at least 24 hours. Importantly, they also found that the drop shows no short-term structural effects on the eye, with only temporary changes in blood flow inside the retina.
Ostrin’s latest research is published in the journal Eye and Vision. It adds to a growing body of vision research from David Berntsen, Golden-Golden Professor of Optometry at the University of Houston, who is co-leading a national $25 million NIH-funded clinical trial to delay the development of myopia in children by using the atropine drops.
Low concentration atropine is widely prescribed to slow myopia progression in children, yet its short-term retinal and choroidal effects remain incompletely understood. Ostrin’s new study evaluated short-term effects of a range of low atropine concentrations on the length of the eye, the blood vessels in the retina and the thickness of the retina and choroid, which sits just behind the retina. These are important measurements because longer eye length is associated with myopia and as it gets longer, the retina and choroid are stretched.
“These findings indicate that a single instillation of atropine does not alter axial length or retinal or choroidal thickness over 24 hours but may transiently affect superficial retinal perfusion in a time-dependent manner,” said Ostrin.
In the double-masked, randomized study, twenty healthy adults received a single instillation of either a placebo or atropine in the right eye during five separate sessions. Researchers then checked the eye structure, thickness, and length in the central retina both one-hour and 24-hours later.
“Characterizing these short-term effects is important for a better understanding of the physiological responses to atropine in clinical and research settings,” said Ostrin who previously published research results of a study investigating the short-term effects of a range of low-dose atropine concentrations on the pupils of young adults. In that study, she found similar results with a single drop of atropine inducing significant changes in the pupils.
Together, the studies indicate that atropine induces early functional and vascular effects in the eye, in the absence of structural change.
“By linking objective ocular responses with subjective visual experience, this work advances our understanding of how atropine works and supports more precise, evidence-based, and individualized approaches to myopia management,” said Ostrin.
NewsMakers
Study: Egg consumption is associated with a lower risk of Alzheimer’s Disease
Compared to never eating eggs, eating at least five eggs per week can decrease risk of Alzheimer’s.

Consumption of eggs is associated with a lower risk of being diagnosed with Alzheimer’s Disease for those 65 years and older, according to researchers at Loma Linda University Health
Eating one egg per day for at least five days a week reduces risk of Alzheimer’s by up to 27%, researchers found.
“Compared to never eating eggs, eating at least five eggs per week can decrease risk of Alzheimer’s,” said Joan Sabaté, MD, DrPH, a professor at Loma Linda University School of Public Health and the study’s principal investigator.
Even less frequent consumption of eggs significantly reduced the risk of Alzheimer’s. Researchers found that eating eggs 1 to 3 times per month had a 17% decrease in risk, while eating eggs 2 to 4 times per week had a 20% decrease in risk, Sabaté said.
The study, Egg intake and the incidence of Alzheimer’s disease in the Adventist Health Study-2 cohort linked with Medicare data, was published last week in the Journal of Nutrition.
Researchers said they embarked on the study because of a substantial knowledge gap in the relationship between modifiable dietary factors and risk of Alzheimer’s disease risk.
Eggs are known to be a source of key nutrients that support brain health. Sabaté said. Eggs provide choline, a precursor to acetylcholine and phosphatidylcholine, both of which are critical for memory and synaptic function, the study stated. Eggs also contain lutein and zeaxanthin—carotenoids that accumulate in brain tissue and are associated with improved cognitive performance and reduced oxidative stress. Eggs also contain key omega-3 fatty acids, and yolks are particularly rich in phospholipids, which constitute nearly 30% of total egg lipids and are essential for neurotransmitter receptor function.
Researchers said they studied the consumption of eggs in visible ways — such as eating eggs in various forms, like scrambled, fried, boiled, etc. — and hidden ways, such as eggs included in baked goods and packaged foods.
The cases of Alzheimer’s Disease in the Adventist Health Study 2 cohort were diagnosed by physicians, according to Medicare records, among the study population of 40,000 subjects. Eligibility was determined using the Medicare Master Beneficiary Summary Files. The average follow-up period was 15.3 years.
The team emphasized that moderate egg consumption should be part of a balanced diet.
“Research supports eggs as part of a healthy diet,” said Jisoo Oh, DrPH, MPH, an associate professor of epidemiology at Loma Linda University School of Public Health and the study’s lead author. “Seventh-day Adventists do eat a healthier diet than the general public, and we want people to focus on overall health along with this knowledge about the benefit of eggs.”
NewsMakers
Telling people they might lose motivates more than telling them they might win, research shows
How managers choose to frame problems directly influences employees’ motivation to speak up at work. For managers, this is an insightful approach for building more open and collaborative teams.

Athletes say they hate to lose more than they love to win. New research finds the same sentiment is shared in organizations.
A Virginia Tech researcher and his colleagues discovered that when managers frame work problems as a potential loss, employees are more likely to take action than when those problems are framed as potential gains. The research also revealed that when the potential loss impacts a larger group, employees are more likely to take action in the form of speaking up to a supervisor in hopes of finding a solution. The findings were recently published in the Journal of Applied Psychology.
For managers, this research suggests that framing work problems as potential losses can influence employees to speak up more.
“Employee voice occurs when suggestions are made to improve organizational functioning,” said Phil Thompson, associate professor in the Pamplin College of Business Department of Management. “From an organizational perspective, the positive outcomes of employee voice include improved performance, effectiveness, and workplace safety. From an employee level, speaking up is positively related to creativity, innovation, engagement, and ethical behavior.”
At its core, this research shows that how managers choose to frame problems directly influences employees’ motivation to speak up at work. For managers, this is an insightful approach for building more open and collaborative teams.
“When managers say, ‘If we don’t get this done, not only will you lose the $5,000 bonus, but everybody in this work group is going to lose a $5,000 bonus,’ it magnifies an employee’s motivation to act in a proactive way,” said Thompson. “This suggests that framing work problems as what will be collectively lost – compared to what can be individually lost – makes employees want to speak up more.”
Thompson was part of a research team led by Jeffery Thomas and Jonathan Booth from The London School of Economics and Mark Bolino from Oklahoma University. Together they analyzed responses from nearly 2,000 full-time employees, MBA students, and employee-supervisor pairs for their experience in situations where work problems were framed as either a gain or a loss. Across three different studies, framing something as a loss yielded employees to voice a work suggestion more.
For example, a manager dealing with a reputational crisis of their team, such as a product quality issue, can frame the problem in a way to spark helpful employee suggestions on how to resolve the issue. For example, instead of saying “if this product has great quality, our company will look really good” a manager saying “if this product is not up to quality standards, our reputation will be damaged” carries more weight for the team. When this reputational risk is shared by everyone, employees are more willing to step forward to help the problem.
In the first study, participants were asked to think about a problem at work that was significant for them. From there, they were randomly assigned to write about the potential losses or gains from that problem. They were also asked to indicate how likely they were to talk about these problems to their supervisor. Participants who reflected on their potential losses showed a 16 percent higher willingness to speak up compared to those who focused on the potential gains.
When it came to the MBA students, they read a fictional performance review scenario where a workplace problem was described. They then rated how willing they would be to speak up about that scenario if they were in the situation. One example suggested that the entire team might fall short of its goals if an issue was not addressed. This specific scenario yielded the most likelihood of speaking up 35 percent more than the scenario’s suggesting that only they would miss their goal, supporting the research’s findings that an employee is more likely to speak up when the loss impacts more people.
The third study looked at employee-supervisor pairings to understand how these relationships play out in the real world. Using pairings from across three industries, employees reported a workplace problem they encountered and their supervisor rated how often that employee spoke up on the job. While the first two studies involved hypothetical scenarios, this real-world evidence showed that employees were 8-10 times more likely to speak up when issues were framed as a potential collective loss compared with a potential collective gain.
“This research is really geared toward managers so they can facilitate and understand how and why their employees will speak up,” said Thompson. “You can talk about the issue, but it always ends in terms of how we frame things.”
-

 Destinations4 weeks ago
Destinations4 weeks agoCoffee-craving with rice meals on the side at Foam Coffee
-

 Wellness4 weeks ago
Wellness4 weeks agoAdding resistance training improves strength and aerobic fitness, better for heart health
-

 Destinations2 weeks ago
Destinations2 weeks agoChecking Cavite’s Lolo Claro’s
-

 Wellness2 weeks ago
Wellness2 weeks agoMidlife fitness linked to longer, healthier lives
-

 NewsMakers2 weeks ago
NewsMakers2 weeks agoTelling people they might lose motivates more than telling them they might win, research shows
-

 NewsMakers2 weeks ago
NewsMakers2 weeks agoYoga practice could reduce blood pressure in people with obesity
-

 NewsMakers4 weeks ago
NewsMakers4 weeks agoStress, BMI, and hormones linked to earlier puberty in girls
-

 Home Care4 weeks ago
Home Care4 weeks agoReduce your home’s vulnerabilities to wildfire